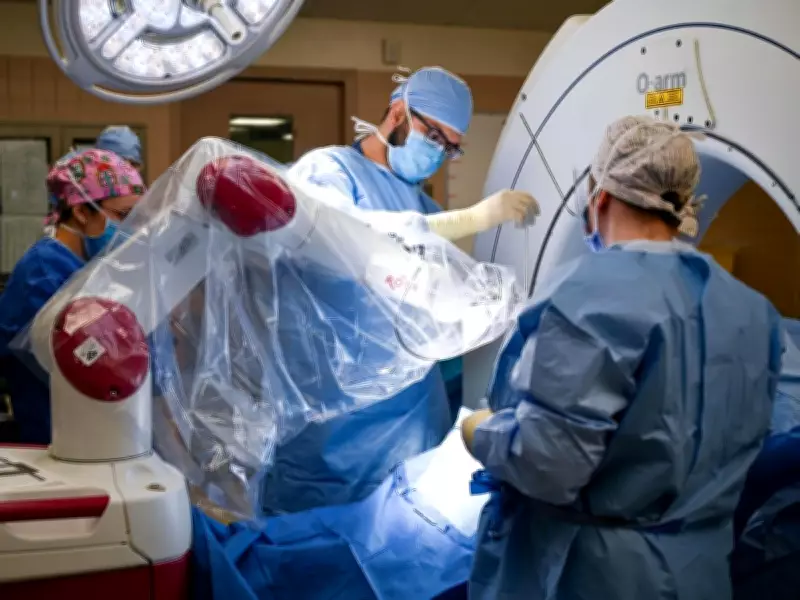
Saskatchewan Woman Awaits Seizure as Province's First Robotic Epilepsy Surgery Patient
Jacky Willmek, a longtime Saskatoon resident and pharmacy assistant, is currently tethered to the wall at Royal University Hospital with ten tiny flexible electrodes inside her skull. She is waiting to have a seizure so a computer can precisely map its location in her brain. Willmek lives with epilepsy that cannot be cured with medication, making her the first person in Saskatchewan to undergo surgery performed by a neurosurgical robot.
Accessing Care Close to Home
Willmek considered transferring her case to Calgary but was able to access this cutting-edge care close to home. The technology launched at RUH with the help of a $1.2 million campaign in 2025, offering a similar timeline to out-of-province options. "It's pretty exciting, because then I can actually have people come visit me. Like, I've had somebody here every day," the 35-year-old said in a phone interview with the StarPhoenix.
More than two weeks out from the robotic surgery, with wires coming out of the left side of her head, Willmek is playing a waiting game—and consuming quite a bit of Netflix. "I feel like I'm somehow putting some pressure on myself, like I need to have a seizure, even though I'm very aware I have no control over that," she admitted. "I wish I did. If only I could make myself."
Robotic Precision for Brain Mapping
The fact that Willmek's surgical team believes her seizures consistently originate from just one part of her brain—the left temporal lobe—made her an ideal candidate as the robotic system's first patient. Dr. Amit Persad, her neurosurgeon, compares the technology to a guarantee of hitting the bull's-eye when inserting electrodes into the brain.
"You can think of the electrodes as being bullets, like we've got to put bullets into the exact right spot ... With the robot, it puts us at the exact right angle and distance that we can just hit bull's-eye every time," Dr. Persad explained. "Putting these electrodes in manually, without the robot, is at least twice as inaccurate, based on studies that we have available."
The result of manual insertion is inferior imaging data and increased safety risks for patients. Thus, relying on the robot has become the standard of care in RUH's seizure investigation unit, with Saskatoon positioned in the "middle of the pack" among Canadian cities adopting this technology.
Minimally-Invasive Procedure with Major Impact
For patients like Willmek—nearly 4,000 people in Saskatchewan live with drug-resistant epilepsy—this minimally-invasive procedure represents a critical step. The surgery takes about an hour and a half in the operating room and serves as a mini-surgery that could enable a larger operation to cure the condition.
Once inside the brain, the electrodes, which resemble bendable millimeter-thin wires with about ten contact points each, collect data to record brain activity. "So we can aim those electrodes to get the most important areas," said Dr. Alexandra Carter, director of the Saskatchewan Epilepsy Program. "... And then that lets us build that 3D map."
This advanced mapping is crucial for identifying the exact origin of seizures, paving the way for potential surgical interventions that could offer lasting relief. The robotic system's ability to place electrodes about as thick as a small blade of grass with unprecedented accuracy marks a significant advancement in neurological care.
As Willmek continues her wait at Royal University Hospital, she remains hopeful that this pioneering procedure will provide the answers needed for effective treatment, all while staying connected to her support network in Saskatchewan.









