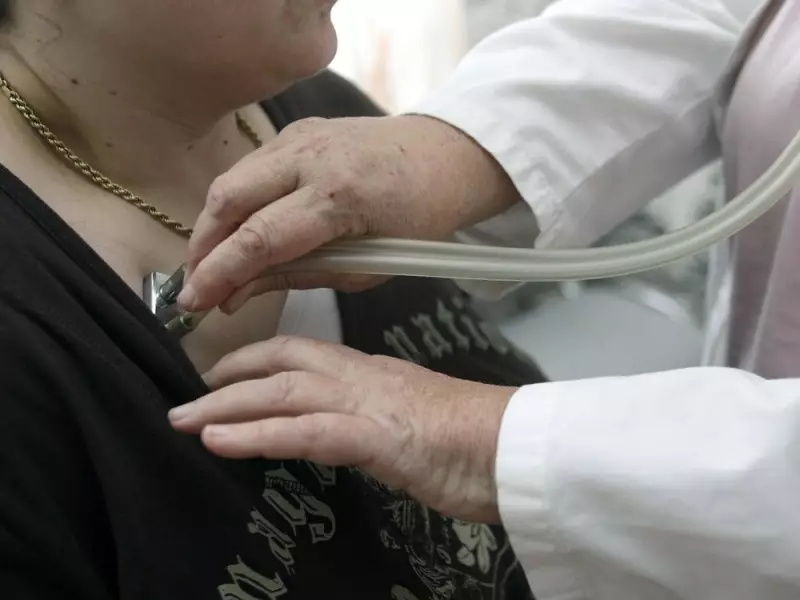
Quebec's healthcare system faces a critical juncture as Bill 2 fundamentally rewrites medical practice rules, raising urgent questions about how much political control a health system can withstand before patient trust completely collapses.
The Intrusion into Clinical Space
According to bioethicist Marie-Josée Potvin, who has over 35 years of experience in healthcare ethics, Bill 2 represents the political equivalent of kicking down the exam-room door. This legislation constitutes a severe intrusion into the clinical space that healthcare workers have dedicated decades to protecting.
What should remain a protected sphere—the intimate, complex encounter between vulnerable patients and their clinicians—is now being reshaped by ministerial targets, algorithms, and automatic sanctions. This transformation threatens the very foundation of medical trust that has long characterized Quebec's healthcare system.
Healthcare Professionals Push Back
The tension reached a boiling point recently when Montreal healthcare workers protested outside Radio-Canada. One family doctor captured the growing frustration with unusual bluntness, comparing the legislation to policies from authoritarian regimes: "This policy, this law—you would think it came out of Cuba, North Korea or the Soviet Union."
Premier François Legault has attempted to reassure the public in financial terms, emphasizing that "there will be no reduction in the Quebec health budget." However, Potvin argues this response reveals a fundamental misunderstanding of the crisis. The issue isn't primarily financial but structural—concerned with the conditions that make quality care possible, not simply the size of budget allocations.
Breaking the Social Contract
At the heart of this crisis lies the weakening of the social contract governing public medicine—a three-way pact binding government, physicians, and the public. This arrangement protects patients by ensuring that government provides fair working conditions, clinicians exercise independent professional judgment, and the public trusts that political or economic pressures won't override what happens in the exam room.
When this delicate balance breaks down, trust collapses completely. While performance targets have pressured this balance for years, Bill 2 introduces unprecedented force. Metrics now intrude aggressively into clinical decisions, with algorithms defining "success" and automatic sanctions looming over healthcare professionals whose choices don't align with prescribed indicators.
The Human Cost of Political Control
Healthcare professionals have adapted for decades—reorganizing, compensating, and absorbing administrative demands to protect what makes medicine effective: listening carefully, assessing risk appropriately, and following fragile patients over time. With mandatory quotas and sanctions now imposed, the space for professional discretion shrinks dramatically.
The Quebec ombudsman has identified deficiencies in service quality as the leading cause of complaints for at least three years—well above access issues, even though "access" serves as the government's primary justification for Bill 2. Clinicians observe the same troubling trend: chronic care fragments, mental health loses continuity, and complex patients become deprioritized.
Each time a political target overrides actual care needs, a silent triage occurs—and the most vulnerable patients lose first.
Restoring the Proper Boundaries
Bioethicists have long noted the paradox of training clinicians: society expects healthcare professionals to practice the medicine they were trained for, while giving them working conditions that make this nearly impossible. Bill 2 sharpens this tension dramatically, normalizing situations where meeting political targets can push clinicians toward choices that conflict with their ethical duties.
Quebec has experienced reform after reform, often well-intentioned yet poorly aligned with the actual demands of patient care. There's a crucial distinction between governing a health system and governing medicine: one manages structures and resources, while the other shapes the intimate encounter where a person seeks both help and hope.
When the exam room becomes an extension of ministerial policy, the social contract that protected both patients and the core of medicine no longer holds.
The solution isn't to completely separate medicine from politics, but to restore the proper boundaries that allow each domain to function effectively. It's time for government and physicians to leave the exam room and return to the negotiation table—to confront the conflict Bill 2 has exposed and establish limits that protect the trust essential to quality healthcare.
This approach represents the only way to redefine responsibility and safeguard the common good that both healthcare professionals and politicians ultimately seek to serve.









